
Unintentionally eating while asleep—what’s behind it and how can you stop? This common concern, known as ‘eating in sleep,’ can be a sign of underlying disorders like SRED or NES. Here, we explain these conditions and provide actionable insights for treatment, without overwhelming medical jargon.
Key Takeaways
Sleep-Related Eating Disorder (SRED) and Night Eating Syndrome (NES) are distinct nocturnal eating disorders with separate characteristics; SRED occurs during sleep, often with no memory of the event, while NES involves conscious eating at night and significant caloric intake post-evening meal.
Diagnosis of nocturnal eating disorders involves a comprehensive review of the individual’s medical and sleep history, and may include tools like the Night Eating Questionnaire (NEQ) and polysomnography to monitor sleep activity and identify specific eating behaviors.
Treatment of nocturnal eating disorders typically combines medication, cognitive behavioral therapy, and lifestyle modifications, alongside preventative measures such as sleep hygiene practices, stress reduction, and regulating the body’s circadian rhythm to lessen nighttime hunger.
Understanding Sleep-Related Eating Disorders (SRED)

Sleep-Related Eating Disorder (SRED) is a paradoxical condition that merges two of the most essential human functions – eating and sleeping. It involves involuntary sleep eating episodes during sleep, with the affected individuals often oblivious to their actions. The peculiarity of this disorder is that eating episodes typically occur during the first few hours of sleep, particularly during transitions between sleep cycles.
The disorder poses significant health risks, as individuals with SRED may consume not just unhealthy food, but also non-food items, posing a risk of ingesting hazardous substances like bleach or coffee grounds. Moreover, the persistent nocturnal eating could lead to refractory obesity and its associated complications.
Identifying Symptoms of SRED
Recognizing the symptoms of SRED is vital in ensuring timely diagnosis and treatment. The disorder is characterized by frequent nocturnal eating episodes that can occur every night or several times a week, and in some cases, even multiple times in a single night.
Intriguingly, individuals with SRED often have little or no memory of their actions, including getting out of bed and eating, during the episodes. The episodes are marked by confusion or an altered state, and the individuals can be difficult or impossible to awaken. These nocturnal eating activities can lead to accidental injuries, such as cuts and burns, due to impaired consciousness, adding another layer of risk to this disorder.
The Connection Between SRED and Other Sleep Disorders
One of the perplexing aspects of SRED is its frequent affiliation with other primary sleep disorders. These associations can significantly disrupt sleep quality. One example is that SRED may be linked to sleep issues, like sleepwalking or restless legs syndrome. These problems can negatively impact the quality of sleep for individuals with SRED. Interestingly, these disorders can run in families and affect multiple members.
When SRED is related to other parasomnias or sleep disturbances, treatment of the associated sleep disorder is beneficial. For instance, if SRED is associated with Restless Legs Syndrome (RLS), treatment with dopamine agonists like pramipexole has been shown to be effective.
Decoding Night Eating Syndrome (NES)

While SRED stands out due to its occurrence during sleep, Night Eating Syndrome (NES) brings a different dimension to nocturnal eating disorders. NES is characterized by a persistent urge to eat during the night and upon waking, contributing to a significant portion of daily food intake occurring after the evening meal or during nighttime awakenings.
Individuals with NES experience sleep disturbances and commonly wake up several times during the night with an uncontrollable need to eat. They are often unable to return to sleep without eating. Moreover, these nocturnal eating episodes typically involve consumption of high-calorie foods, resulting in over a quarter of their daily caloric intake being consumed after the evening meal.
How NES Differs From Binge Eating Disorder
While NES and binge eating disorder might seem similar due to excessive eating, they have distinct characteristics. NES is characterized by a delayed circadian pattern of food intake, contrasting with binge eating disorder where individuals consume large amounts of food in a short time period.
Moreover, unlike binge eating disorder, NES does not necessarily involve the consumption of large amounts of food nor the experience of losing control during eating episodes. Patients with binge eating disorder are often preoccupied with eating, weight, and body shape, experiencing a loss of control during eating episodes. This differs from NES, where individuals commonly eat average or smaller portions at night without such concerns.
The Impact of NES on Daily Life
The repercussions of NES extend far beyond disturbed sleep and late-night snacking. It can lead to obesity and associated health issues such as type 2 diabetes and heart disease, often resulting from the consumption of high-calorie foods at night.
The nocturnal eating episodes in NES often involve high-calorie but low-nutrient foods, leading to poor nutrition which further exacerbates weight gain and health complications. The disrupted sleep architecture from NES can lead to non-restorative sleep and pronounced daytime fatigue, hindering an individual’s ability to function during the day. Moreover, altered eating patterns such as skipping breakfast and eating less during the day promote a cycle of nighttime hunger and can increase the risk of health issues like diabetes and high blood pressure.
Diagnosis and Professional Insight
Diagnosing nocturnal eating disorders such as SRED and NES involves an in-depth analysis of the patient’s medical history, sleep history, and certain diagnostic tools. Discussing the patient’s complete medical history and concerns about food intake or meal patterns with a doctor is the first step to diagnosis.
While SRED is diagnosed based on recurrent episodes of involuntary eating and drinking during the main sleep period, NES diagnosis involves evaluating the patient’s health issues, mood, stress levels, and mental health. A comprehensive evaluation for diagnosing NES and SRED typically includes a detailed sleep history, a complete medical and psychiatric history, and polysomnography with synchronized video and a full EEG montage.
Utilizing the Night Eating Questionnaire (NEQ)
The Night Eating Questionnaire (NEQ) is a tool used to assess if a person’s feelings and behaviors are consistent with NES. The NEQ helps in diagnosing NES and assessing unusual eating behaviors related to sleep by highlighting patterns in food intake, timing, and the individual’s awareness and emotions surrounding eating episodes.
By providing a comprehensive picture of a person’s nocturnal eating patterns, the NEQ aids healthcare professionals in accurately diagnosing NES and formulating effective treatment strategies.
The Role of a Sleep Study in Identifying SRED
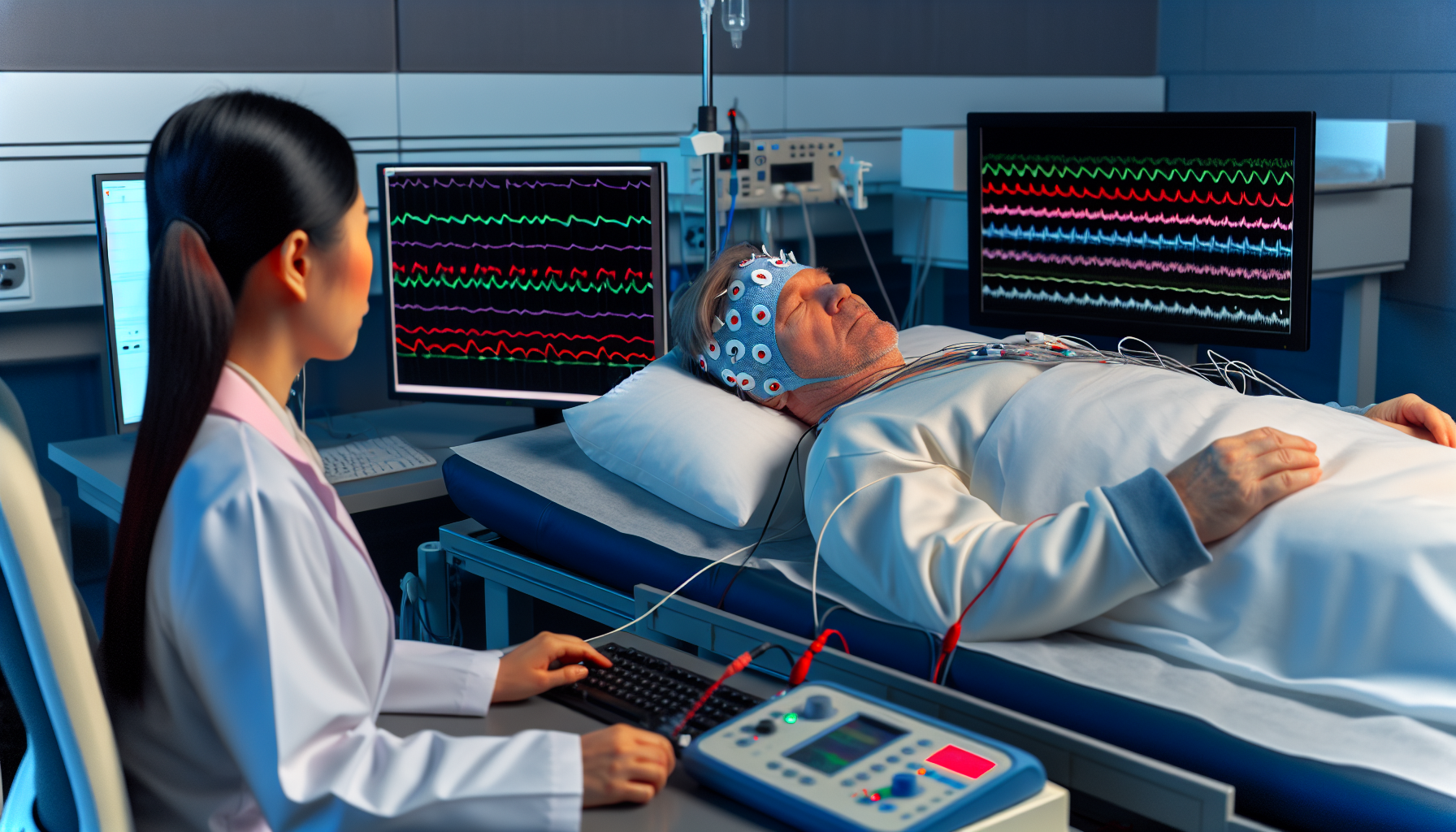
Sleep studies are instrumental in diagnosing SRED. Polysomnography (PSG), a type of sleep study, is considered the gold standard for detecting sleep disorders and can help identify SRED by recording:
Brain waves
Muscle activity
Breathing
Eye movements during sleep
PSG can distinguish SRED from other sleep disturbances and eating disorders by utilizing parameters such as electroencephalography and by observing the patient’s sleep behavior through video recordings. Video-polysomnography (v-PSG) is particularly instrumental in capturing episodes of nocturnal eating, providing concrete evidence of eating behaviors during partial wakefulness or specific sleep stages for the diagnosis of SRED.
Treatment Strategies for Nocturnal Eating Issues

Treating nocturnal eating disorders involves a holistic approach that combines medication, cognitive behavioral therapy, and lifestyle changes. Selective serotonin reuptake inhibitors (SSRIs) at mean dosages of 20 to 30 mg/day are the first-line treatment for idiopathic Sleep-Related Eating Disorder (SRED). Alternate medication options for SRED include topiramate and clonazepam.
For Night Eating Syndrome (NES), a combined approach of antidepressant medications and cognitive behavioral therapy is commonly employed along with strategies to normalize sleep and eating patterns. Lifestyle changes, such as creating a safe kitchen environment and removing harmful substances, also aid in managing SRED.
Medication Options: SSRIs and Beyond
In terms of medication for SRED, Selective serotonin reuptake inhibitors (SSRIs) are often used as a first-line treatment, with common dosages ranging from 20 to 30 mg/day. However, every individual is unique, and what works for one may not work for another.
For those who may not respond to SSRIs, alternative options include topiramate and clonazepam. Pharmacotherapy for sleep-related eating disorders, guided by mental health professionals, includes using medications such as sertraline and topiramate and has shown to be effective in some cases.
Cognitive Behavioral Therapy (CBT) and Lifestyle Interventions
In addition to medication, Cognitive Behavioral Therapy (CBT) is a key component in the treatment of nocturnal eating disorders. For NES, CBT targets the misguided belief that eating is necessary for sleep and helps individuals transition to consume more of their food intake earlier in the day.
Behavioral strategies for SRED can include improving awareness of nocturnal eating and enhancing sleep quality by establishing a safe and proper sleep environment, combined with stress management techniques.
A well-designed meal plan advised by a dietitian or nutritionist is crucial for individuals with SRED to meet nutritional needs and possibly lessen nighttime eating episodes.
Preventative Measures and Healthy Habits

Preventative measures hold equal importance to treatment strategies in managing nocturnal eating disorders. Establishing proper sleep habits can be facilitated by following a sleep hygiene plan, which includes a consistent sleep schedule and pre-sleep routine. Avoiding substance abuse is a key preventative measure against nocturnal eating disorders, as substances can disrupt sleep patterns and impact eating behaviors.
Lifestyle changes such as regular meal timing and avoiding late-night snacks can also be beneficial in preventing the development of nocturnal eating disorders. Additionally, practicing stress reduction techniques like mindfulness, meditation, or yoga may contribute to better sleep quality and reduce the likelihood of nocturnal eating episodes.
Importance of Circadian Rhythm Regulation
For individuals battling nocturnal eating disorders, regulating the body’s internal clock, or circadian rhythm, can be a significant turning point. Structured eating and sleeping times can help regulate the circadian rhythm, which could help distribute food intake throughout the day and decrease hunger at night.
Eating more calories in the morning as opposed to later in the day could significantly decrease the risk of developing overweight or obesity, underlining the significance of aligning meal timing with the body’s circadian rhythms. Meal plans that are aimed at preventing sleep-related eating disorders should include sufficient amounts of protein and fiber to ensure satiety and lessen the urge for eating at night.
Additionally, adopting a regular sleep schedule and ensuring adequate sleep can reduce the likelihood of nocturnal eating episodes, as it helps you fall asleep without disruptions.
Addressing Daytime Dieting and Stress
Daytime dieting and stress are two significant factors that can exacerbate nocturnal eating disorders. Causes of NES can include dieting and stress, leading to overcompensation at night.
Establishing a regular meal pattern during the day helps control appetite and may reduce the likelihood of nighttime eating. A high-protein diet can decrease cravings and reduce the desire to eat at night due to prolonged satiety. Planning meals and healthy snacks in advance can prevent impulsive eating, which is associated with higher calorie intake and weight concerns.
Weight management strategies and exercise can address SRED, and food diaries can increase mindfulness of eating habits.
Coping Mechanisms and Support Systems
Coping with nocturnal eating disorders can be challenging, but various mechanisms and support systems can ease this journey. Individuals with Night Eating Syndrome (NES) may experience social isolation and embarrassment, impacting their social interactions and relationships.
NES can lead to:
Decreased work performance
Concentration issues
Disrupted sleep
Psychological stress
Those suffering from sleep apnea and sleep-related eating disorders, including sleep eating disorder, may contend with secondary psychological issues like anxiety and depression, which could drive nocturnal eating behavior and contribute to other eating disorders.
Behavioral interventions targeted at associated psychological factors such as anxiety or depression can be effective coping mechanisms in reducing the frequency of nocturnal eating episodes.
Developing a Food Diary and Meal Plan
Developing a sleep and food diary can be an effective strategy for managing nocturnal eating disorders. By tracking all food intake, including during nocturnal episodes, individuals can identify patterns and triggers, providing valuable insights that can aid in managing the disorder.
A food diary can also provide insights into dietary habits that may need to be adjusted. In addition, a structured meal plan, including balanced meals throughout the day, can regulate hunger and possibly reduce the urge to eat at night.
Seeking Help from Mental Health Professionals
Seeking help from mental health professionals can be beneficial for individuals struggling with nocturnal eating disorders. Night Eating Syndrome (NES) is often connected with mental health concerns such as depression or anxiety, which can worsen at night, leading to feelings of shame and guilt. Having night eating syndrome diagnosed by a professional can help address these issues effectively.
Mental health professionals hold a significant role in tackling any underlying anxiety disorders or depression that may act as catalysts for the development of sleep-related eating disorders. Therapy sessions can create a supportive setting where individuals with SRED can explore their emotional state, gaining insights into triggers and addressing associated feelings of shame, guilt, or loss of control.
Working with mental health experts assists in formulating individualized coping mechanisms that effectively manage stress and emotional triggers, key factors involved in nocturnal eating episodes.
Summary
In conclusion, nocturnal eating disorders such as Sleep-Related Eating Disorder (SRED) and Night Eating Syndrome (NES) are multifaceted conditions that require comprehensive understanding, proper diagnosis, and effective treatment. They not only disrupt sleep and eating patterns but can also pose significant health risks and affect an individual’s quality of life.
However, with the right knowledge, professional guidance, and coping strategies, these disorders can be effectively managed. From maintaining a food diary and regular meal timing to seeking help from mental health professionals, there are numerous ways to navigate this journey. Remember, you are not alone in this, and with proper help, you can regain control over your sleep and eating patterns.
Frequently Asked Questions
Why am I eating in the middle of the night?
It’s possible that you have a circadian rhythm disorder, causing your body to release hormones that make you feel hungry and alert at night instead of during the day.
What are the side effects of sleeping immediately after eating?
Sleeping immediately after eating can lead to worsened indigestion symptoms, weight gain, and disruptions to sleep patterns. However, some foods like protein shakes and kiwi fruit can have positive effects on muscle growth and sleep.
What is Sleep-Related Eating Disorder (SRED)?
Sleep-Related Eating Disorder (SRED) is characterized by involuntary eating during sleep, often occurring during the first few hours of sleep. It is common for affected individuals to be unaware of their actions during these episodes.
How is Night Eating Syndrome (NES) different from binge eating disorder?
Night Eating Syndrome (NES) is different from binge eating disorder because it involves a delayed circadian pattern of food intake, unlike binge eating disorder where individuals consume large amounts of food in a short time period. It does not necessarily involve the consumption of large amounts of food or the loss of control during eating episodes.
How are SRED and NES diagnosed?
SRED and NES are diagnosed through an evaluation of the patient’s medical history, discussion of food intake, and a comprehensive evaluation including a detailed sleep history. A doctor typically performs this evaluation to diagnose these conditions.
Why am I eating in the middle of the night?
The circadian rhythm is our bodies natural clock that regulates the amount of time it takes for the person to get tired. NES is not functioning as normal. Your body produces hormones to help with your hunger and alertness.
